Electronic safety-netting (E-SN) toolkit for EMIS web by the North Central London (NCL) Cancer Alliance
Safety-netting in primary care is central to how clinicians and GP practices manage risks such uncertainty in diagnosis and management in daily practice, especially in the context of cancer care provision. Yet, safety-netting is not uniformly understood and is applied in a variable manner across primary care. In the cancer field, safety-netting has been advocated to improve earlier cancer detection, by reducing avoidable delay, which ultimately improves the cancer outcomes and patient experience. Numerous system and local level cancer audits and significant event analyses into cancer diagnoses, reveal the intricate steps in the pre-cancer diagnosis pathway, and highlights areas of missed opportunity that could be improved at a system and healthcare professional level. Examples are patients not returning for follow up or diagnostics not being performed or significant findings not being followed up or actioned. National guidance and policies such as NICE guidance NG12 for suspected cancer: recognition and referral and the Cancer taskforce report have been significant drivers for organisations to implement improvements to current safety netting methods. The use of high quality safety-netting systems applied systematically in primary care would support more robust management of uncertainty to minimise delays and reduce misses.
Situation
Safety-netting in principle is simple and supports patient safety and patient experience at its heart, by providing information for patients and organising follow-up after contact with a health professional. But its application in practice has been challenging, inconsistent and varied. Patients with possible cancer who present to primary care may often have non-specific symptoms and the diagnostic uncertainty poses the biggest management risks. Multitude of cancer case reviews and national drivers have exposed the complexities and fragilities in navigating through a suspected cancer pathway and priority areas for improvement include higher quality safety netting.
Aspiration
The key aspiration was to elevate the quality of safety-netting in primary care in the cancer context but go beyond guidance to deliver solutions. The broad picture of methods of safety netting spanned verbal, written and electronic and at the start of this project there was no tangible offer of a systematic and electronic way to follow up patients being investigated for cancer or being followed up with cancer in primary care.
Solution and impact
The key aim was to develop a streamlined safety netting solution and this was achieved through developing the electronic safety-netting (E-SN) toolkit which was embedded into the primary care electronic health and record system (EHRS) – EMIS Web.
This toolkit is utilises technical features within EMIS Web already, to enable practices to track patients who are being investigated for cancer and/or having follow-up care after a cancer diagnosis or treatment.
The toolkit has a clinical and administrative interface. Clinicians would use the template interface and administrative staff would lead on the tracking and follow up aspects. The template has read coded events tagged to diary entries, which are like time reminders for an action set. The events could be urgent suspected cancer referrals, direct access to ultrasound, or following up of a patent with vague abdominal symptoms. The time reminders are there to ensure the events, such as referrals or tests requested, are followed up. All open reminders will show up on the ‘regularly run’ searches and also will have pop-up reminders when the patient’s record is accessed by the practice staff. The running of searches leads to specific tasks such as follow up calls, reminders, test tracking and action closures.
The implementation of E-SN in the practice requires a systematic whole-practice approach to safety-netting with clinical and administrative leadership. It is not person-dependent and there is a clear audit of the events tracked.
Functionality
In June 2018, EMIS Web published the toolkit centrally, so that all practices in the UK who are using EMIS Web can access it within the current system. The toolkit uses functionalities that are familiar to many primary care professionals (for example, diary entries and searches) which make it accessible and understandable. As it is embedded within EMIS Web, practices do not have to purchase any additional software or tools to use it.
Capabilities
- Tracking of clinical events related to cancer and other conditions
- Pop-up alerts that remind users that the patient is being tracked when the patient’s record is opened
- Events that need to be followed up will appear on a search log once the date associated with the clinical event or tracked event has expired
- The safety-netting loop can be completed (complete diary entry) once the user is happy the event has been recalled by the patient satisfactorily

Scope
The E-SN toolkit is built into EMIS Web and is for GP practices and their teams to use. E-safety netting can be at a practice level or could be implemented at scale, for example Primary care network (PCN) or GP federation. At scale models need to have the administrative capacity and support to ensure the system functions optimally.
Key learning points
The improvement journey and resulting service evaluation has shown that the toolkit is user-friendly, with high degrees of acceptability in primary care, and has made positive improvements to safety-netting processes in practices.
The wider learning covers the complex nature of promoting a new way of working in primary care, without commissioning or contractual levers. The toolkit’s simple and integrated interface had extensive appeal and wider applicability beyond cancer tracking.
Successful adoption of this systematic way of working requires whole-practice engagement, with administrative and clinical ownership and leadership.
Early adopters were crucial to the improvement-at-scale journey, as was the wider strategic support from Macmillan.
Key figures/quotes
Users were asked: ‘Will you continue to use this safety netting tool going forward?’
User responses:
- 96% said ‘Yes’ they would continue to use the tool
- 2% said ‘No’
- 2% did not respond
The service evaluation highlights that at the initiation workshops, 89% of attendees felt that the toolkit was a more robust method of safety netting when compared to their current system.
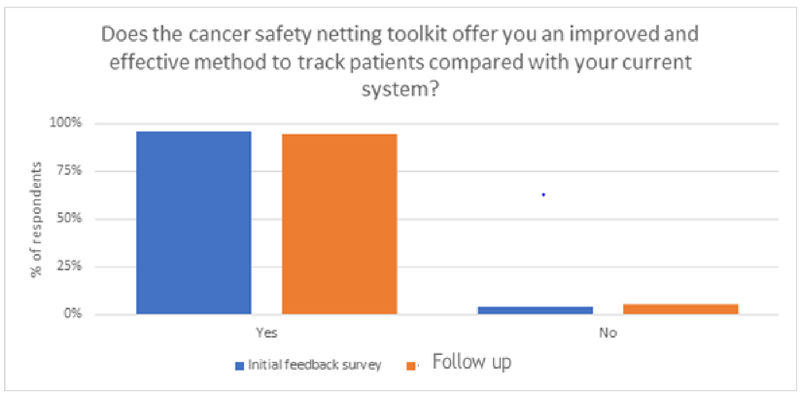
4 months after implementing the system, 93% of pilot practices indicated that the Electronic Safety Netting Toolkit offered an improved, more robust safety netting system compared to their previous systems.
“Just to say, what you have done from start to finish with this is awesome and has had a wide-reaching patient impact. A big thank you from me.”
Tania Anastasiadis, GP, Tower Hamlets and Macmillan GP and GP advisor for Tower Hamlets (July 2020)
“The safety netting toolkit is live in my practice and, not only was it easy to apply, but the benefits for clinicians and patients alike were evident immediately. I am sure clinicians will quickly realise its potential in tracking and safety netting patients of concern and will welcome the fact that this can be done collaboratively with other colleagues within the practice team.”
Dr Rosie Loftus, joint chief medical officer, Macmillan Cancer Support (August 2018)
“We have been using the electronic safety netting toolkit since late 2018. We have to say it has been extremely effective. We didn't have any safety-netting tools in place beforehand. Going forward, the diagnostics section will be particularly useful as primary care access to direct access investigations has been disrupted by the COVID-19 pandemic.”
Dr Baber Qadir, Romford GP and practice cancer lead, North Street Medical Care (March 2021)
“An advantage is that you can tweak it in any way you like to make it fit your individual team. We are a small practice and we tweaked it to attach a report to the tool to use it beyond cancer, for example, chronic kidney disease... which allows us to book appointments a few months in advance and send them a reminder.”
Dr Kanicka Rai, GP and cancer lead for Barking, Havering and Redbridge University Hospitals NHS Trust (March 2021)
Find out more
Find out more about the safety-netting from NCL Cancer Alliance
Read about the CDS tool on the RCGP website
Key contact
Dr Afsana Bhuiya, cancer GP at North Central London Cancer Alliance
Disclaimer
These case studies summarise user and patient experiences with digital solutions along the relevant care pathway. Unless expressly stated otherwise, the apps and digital tools referenced are not supplied, distributed or endorsed by NHS England or the Department of Health and Social Care and such parties are not liable for any injury, loss or damage arising from their use.
All playbook case studies have either passed, or are currently undergoing the Digital Technology Assessment Criteria (DTAC) assessment.
Please note the full legal disclaimer: NHS England playbook disclaimer