A digital recovery platform for severe mental illness
Severe mental illness (SMI) refers to an enduring mental illness that is often so debilitating that the person’s ability to engage in functional and occupational activities is severely impaired (Public Health England, 2018).
NHS City and Hackney Clinical Commissioning Group define SMI as people with long-term severe mental health needs covering: psychotic disorders, bipolar disorders, personality disorders and severe mood disorders. City and Hackney has the third largest SMI population in England with an estimated 12,000 people experiencing psychotic, personality or severe mood disorders.
Within the NHS, provision at City and Hackney community-based support for SMI includes specialist psychotherapy service, community mental health teams (also known as recovery teams) and crisis services. Voluntary sector providers (The Advocacy Project and Core Sports) are also key services involved.
Situation
Around half of individuals in City and Hackney presenting with SMI sit within primary care. For these individuals there used to be little in terms of structured support apart from that provided by voluntary sector organisations, who lacked connectivity with primary care or secondary care information systems.
Of the remaining half who enter secondary care, only 16% received psychological treatments lasting more than 12 weeks and was a substantial waiting list. Staff capacity was an issue, with 19.3 whole time equivalent staff delivering 1,000 secondary care psychological treatments per year.
In 2018, feedback from service users identified key concerns with recovery plans:
- Difficulties were experienced by patients with accessing the care plans
- The process was described as a one-off assessment or tick-box exercise
- There was a lack of ongoing review and change
- Plans were not shared between services leading to patients feeling like they were repeating themselves
- Planning stopped at discharge from secondary care leading to a support vacuum.
Aspiration
The aspiration was to provide an integrated and interactive patient-led method for individuals with SMI to access timely support from all relevant professionals.
Solution and impact
In 2019, elements of the platform were trialed, including combining personal health budgets with recovery care plans and combining psychological therapy apps with personal logs and outcome measures. In 2020, these elements were brought together using the ‘Patient Knows Best’ platform to create a comprehensive digital recovery platform. The platform provides an interactive toolkit for planning and maintaining recovery by supporting an ongoing recovery plan that service users take with them after discharge and can transfer between organisations.
A key feature of the support offered to patients with SMI at City and Hackney is the development of individual recovery goals as part of a recovery care plan. The plan is developed with support from primary and secondary care specialists. Discharge from secondary care is considered a patient achievement, which is a prominent goal in the recovery care plan.
In addition to providing patient autonomy and choice, the platform cuts out long psychological therapy waiting times.
Since the pilot began in 2019, 569 people with SMI have accessed digital platforms (either prototypes or the final version). Of these:
- 424 have accessed personal health budgets (this enables them to receive resources to achieve their recovery goals)
- 145 have used psychological therapy apps
- 51 patients used the PKB platform with sports programmes in the voluntary sector organisation Core Sport.
Of those who completed engagement with the digital platform for over 9 months:
- 66% fully achieved their goals and 14% partially achieved them
- 72% showed improvement and 52% showed significant improvement on the Department of Health-recognised recovering quality of life (ReQuol) psychometric measure
Support has been provided to overcome any digital poverty issues:
- personal health budgets are available to connect people who would benefit from digital services but can not afford digital devices
- the digital devices they receive are pre-loaded with the platform and health and wellbeing apps
- 222 people connected across the digital divide through personal health budgets: 63 laptops, 146 phones, 13 tablets
- 69 service users received digital training to help them use the platform
- 36% African and Caribbean Heritage community access the service (above the population segment percentage, which is 20%)
Functionality
The digital platform is provided by Patient Knows Best. It serves as a landing site for key resources to support an individual with SMI and those supporting them with their recovery.
The platform provides patients with a digital planning toolkit to assist their recovery. To support this, the system links to specific pieces of information on provider information systems so that this flows onto the platform and the patient and people involved in the patient's care can see it if the patient gives permission. This includes the patient’s care plan, their risk plan, assessments and patient rated outcome measures (such as Dialogue and ReQoL10), appointments, diagnosis, medication and allergies, and the patient’s personal health budget.
Capabilities
The aim of the digital recovery platform is to provide service-user autonomy through choice: patients choose what support they want around them and the platform provides a planning toolkit to assist recovery.
Choices include:
- setting goals and steps to achieve goals
- who to share information with
- when and who to ask for help
- fitness apps
- more than 50 therapy and wellbeing programmes
Scope
The Digital Recovery Platform is an integrated and interactive planning toolkit to support individuals with SMI to access support across organisations such as primary, secondary, social and voluntary care in order to plan and maintain their recovery. The advantage of the platform is that it can be used by the patient as regularly as they like in any location. Service users with severe mental illness have stated that they value the fact that they can use it on a daily basis and at home or wherever they are as it helps them get through the day.
Key learning points
The team were surprised by the enthusiasm for using a digital platform among people with severe mental illness. Service users reported that they liked the freedom of choice and the sense of autonomy. However they were also clear that they did not like something that felt too medical or clinical and not mental health specific, and that they valued something that was intuitive to use.
Key figures/quotes
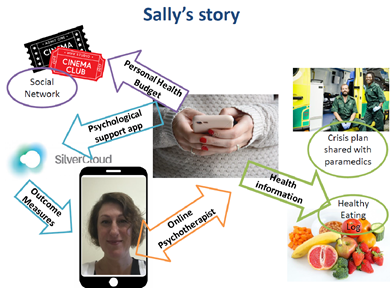
Sally’s story
Sally has significant mental health problems. She has had numerous admissions and felt excluded from most healthcare services.
Sally had found her care plan helped her hold herself together and she had the care plan laminated.
“I had to ensure that I was carrying the document wherever I went, hope that the bag I had with me was not stolen from me while I was dissociative.”
However having a laminated plan meant the document was static rather than dynamic and interactive and there was always the risk of it being lost or stolen. The platform that City and Hackney have developed means that Sally has a ‘virtual backpack’ with immediate online access to her:
- care plan
- crisis plan
- SilverCloud therapies
- personal health budget team’s online resource packages
Sally can message her therapist, update plans, share resources and share information with other services/carers/family.
“I was brought up to be not seen and definitely not heard. Due to this I was left completely unable to ask for any help regardless of the situation.
[This digital platform] has given me the ability to be as self caring as possible for the first time. I am no longer so reliant on my daughter and a few other people to speak for me and access care for me on my behalf. I feel that I am not alone in self caring as I am doing it with the back-up of the professionals who know me very well.
Health professionals who do not know me and the problems I face, have become accessible to me for the first time in my life. I am now able to access care in a way I have never been able to before.”
André’s story
André couldn’t afford a smartphone but received one through a personal health budget, giving him access to the digital platform. He set recovery goals on his recovery care plan on the platform: to become fit and gain confidence and employment skills. He has been discharged into primary care where he continues to access the platform and is an active member of the platform design meetings. He is also enrolling on a tennis coaching course which he hopes will give him employment skills. He has also gained confidence.
“When the pandemic hit, I found it hard. Without the new phone I would not have felt connected. I am the fittest I have been and exercise more during the week than I have ever done! My confidence has grown. I feel it has enabled me to have a voice and be listened to.”
The screenshot below shows André’s Fitbit which was also purchased through a personal health budget and is integrated onto the platform.

Find out more
Find out more about personal health budgets
More about severe mental illness and physical health inequalities
Download the development and validation of the recovering quality of life (ReQoL) outcome measures (PDF, 1.70MB)
Key contact
Dr Miriam Grover, principal cognitive psychotherapist and safeguarding adults manager for SPS, City and Hackney Specialist Psychotherapy Service (SPS)
Dan Burningham, mental health programme director, NHS City and Hackney Clinical Commissioning Group
Supplier : Patients Know Best
Disclaimer
These case studies summarise user and patient experiences with digital solutions along the relevant care pathway. Unless expressly stated otherwise, the apps and digital tools referenced are not supplied, distributed or endorsed by NHS England or the Department of Health and Social Care and such parties are not liable for any injury, loss or damage arising from their use.
All playbook case studies have either passed, or are currently undergoing the Digital Technology Assessment Criteria (DTAC) assessment.
Please note the full legal disclaimer: NHS England playbook disclaimer